Colonoscopy Preparation Timeline Handbook. Episode 4:
T-5 Days - Implementing Medication Changes
Introduction.
Welcome back to our Colonoscopy Preparation Podcast series. I’m Bimal Maharjan, here to guide you through these pivotal days as your procedure approaches. As we enter T-5 days, our focus intensifies on fine-tuning your medication regimen.
Series Overview:
Our podcast series is designed to guide you through each stage of your colonoscopy preparation with detailed, actionable advice. Today, at T-5 days, we focus specifically on the crucial adjustments needed for your medications, ensuring everything is perfectly aligned for your upcoming procedure.
Recap of T-7 Days and Introduction to T-5 Days:
In our last episode, we discussed the adjustments necessary at T-7 days, emphasizing medication management and logistical planning. While T-5 continues on this theme, today's focus shifts more narrowly to ensuring your medications are perfectly calibrated to minimize any risks during your colonoscopy. This episode builds on the previous discussions but dives deeper into the specifics of medication timing and emergency planning.
Overview of Today’s Episode:
In this episode, we’ll explore the precise adjustments you should make to your medications, including how to manage over-the-counter meds and prescription drugs in the days immediately leading up to your colonoscopy. We'll provide detailed examples of how to adjust common medications like insulin, blood thinners, and anti-inflammatories, and discuss the critical importance of coordinating these changes with your healthcare team. We'll also cover how to handle emergency medications on the day of the procedure, ensuring you’re prepared for any situation.
Stay with us, and by the end of this episode, you'll have a clear, actionable plan for managing your medications in the final days before your colonoscopy. We're here to help you navigate these adjustments with confidence, ensuring a smooth and safe procedure.
General Medication Adjustments
Q1: Which medications should I adjust, and how, as I approach the colonoscopy date?
Adjusting medications correctly is essential to minimizing risks such as bleeding, electrolyte imbalances, and interactions with anesthesia. Here’s a focused approach to managing your medications:
Blood Thinners:
Examples: Warfarin, clopidogrel, aspirin.
Adjustment: Most patients will need to stop taking these medications 5 to 7 days before the procedure to reduce the risk of excessive bleeding. Your healthcare provider might replace them temporarily with a different form of anticoagulation, often referred to as 'bridging therapy', depending on your risk of blood clots.
Diabetes Medications:
Examples: Insulin, metformin, sulfonylureas.
Adjustment: Insulin doses may need to be reduced to accommodate the changes in your diet during the bowel prep. Oral medications like metformin might be paused on the day before and the day of the procedure to prevent complications such as lactic acidosis, especially since you'll be fasting.
Anti-inflammatory Drugs:
Examples: Ibuprofen, naproxen.
Adjustment: These should generally be discontinued several days before the procedure to decrease the risk of gastrointestinal bleeding.
ACE Inhibitors and ARBs:
Examples: Lisinopril, losartan.
Adjustment: These medications might be paused on the day of the procedure, particularly if you're instructed to restrict your fluid intake, to avoid low blood pressure during anesthesia.
Other Medications:
For specific conditions: Such as those for heart, lung, thyroid, or psychiatric conditions, continue as prescribed unless specifically advised otherwise by your doctor.
Herbal Supplements and Vitamins:
Examples: Vitamin E, fish oil, ginkgo biloba.
Adjustment: Discontinue these supplements at least a week before the procedure to reduce the risk of bleeding.
It’s crucial to have a detailed discussion with your healthcare provider about each medication you're taking. Provide them with a comprehensive list of all your medications, including over-the-counter drugs and supplements, so they can guide you on which specific ones to adjust and how to do so safely.
Q2: How should I manage over-the-counter medications I typically take for pain, allergies, or sleep?
Pain Medications:
Typical OTCs: Aspirin, ibuprofen, naproxen (NSAIDs).
Management: Stop taking NSAIDs at least 5-7 days before your colonoscopy to reduce the risk of bleeding. If you need pain relief, acetaminophen (Tylenol) is a safer alternative as it doesn’t have the blood-thinning effects of NSAIDs.
Allergy Medications:
Typical OTCs: Antihistamines like loratadine (Claritin), cetirizine (Zyrtec), and diphenhydramine (Benadryl).
Management: Most non-sedating antihistamines can be continued as they do not affect the colonoscopy. However, if you use sedating antihistamines like diphenhydramine, consider consulting with your healthcare provider as these can interact with the sedatives used during the procedure.
Sleep Medications:
Typical OTCs: Melatonin, diphenhydramine-based sleep aids (e.g., Tylenol PM).
Management: If possible, avoid taking sleep medications the night before your colonoscopy. Sedative ingredients, particularly in diphenhydramine-based products, may enhance the sedative effects of anesthesia drugs used during the procedure. If sleep is a concern, discuss non-medication strategies with your doctor or consider using melatonin which has fewer interactions.
Key Considerations:
Always review your usage of OTC medications with your healthcare provider during the pre-procedure consultation. This review should include all supplements and non-prescription drugs you routinely use.
Ensure you mention any OTC medications during your pre-anesthesia evaluation, as these can interact with anesthesia drugs and affect your response to the sedative agents.
Proper management of your OTC medications is a critical aspect of preparing for a colonoscopy. By carefully adjusting your intake of pain relievers, allergy medications, and sleep aids, you help ensure a safer procedure with minimal risk of complications. Always consult with your healthcare provider for personalized advice tailored to your specific health needs.
Heart Conditions
Q3: Should I make any dose modifications to my heart medications, including blood pressure and heart rhythm meds?
When preparing for a colonoscopy, it's essential to maintain stable heart function, which often depends on consistent medication. Here’s how to approach any necessary adjustments:
Blood Pressure Medications:
Typical Medications: ACE inhibitors, beta-blockers, diuretics, calcium channel blockers.
Management: Generally, you should continue taking your blood pressure medications as usual to maintain cardiovascular stability. However, some medications, like diuretics, which affect fluid and electrolyte balance, might need to be adjusted to prevent dehydration due to the colonoscopy prep.
Heart Rhythm Medications:
Typical Medications: Antiarrhythmics such as amiodarone, digoxin.
Management: These medications should generally be continued without alteration to avoid any potential for arrhythmia. However, the specific conditions of your heart health might necessitate adjustments, which should be done under close medical supervision.
Anticoagulants (if applicable):
Typical Medications: Warfarin, direct oral anticoagulants (DOACs) like apixaban or dabigatran.
Management: Modifications or temporary cessation might be required depending on your risk factors for thrombosis versus bleeding. Bridging therapy with heparin could be necessary if stopping anticoagulants.
Contact Your Cardiologist: It is critical to consult with your cardiologist or healthcare provider who manages your heart medications well before your procedure date. They can provide specific instructions based on your cardiovascular health and the types of medications you are taking.
Pre-procedure Consultation: During your pre-procedure consultation, discuss your entire medication regimen, including any over-the-counter drugs or supplements that could interact with your heart medications.
Medication List Review: Bring a complete list of your medications to your consultation. This list should include all prescription medications, over-the-counter drugs, and supplements, along with their dosages and how often you take them.
Adjusting heart medications in preparation for a colonoscopy is a delicate balance designed to maintain heart health and prevent procedural complications. Direct communication with your cardiologist is crucial to tailor these adjustments to your specific needs, ensuring a safe and successful colonoscopy outcome.
Kidney Conditions
Q4: Are there specific considerations for adjusting medications if I have reduced kidney function or am on dialysis?
For those of you managing kidney conditions, it's crucial to adjust your medications in a way that accommodates your reduced kidney function or dialysis schedule. Kidney health significantly impacts how your body processes medications, including those used during a colonoscopy prep.
Adjustment Guidelines:
Water-Soluble Medications: These may need dosage adjustments or timing changes to prevent accumulation in the body, particularly if your kidney function is compromised.
Electrolyte Balance: Medications that affect electrolyte levels must be managed carefully to avoid imbalances that could complicate both your kidney condition and the colonoscopy procedure.
Dialysis Patients: Timing your medication around your dialysis sessions is essential, as some medications might be removed or their effectiveness reduced by dialysis.
Action:
Consultation with Nephrologist: It’s imperative to discuss all your current medications with your nephrologist, who can make specific recommendations based on your level of kidney function and dialysis needs.
Medication Review: Bring a list of all your medications to your appointment, including over-the-counter drugs and supplements, to ensure all aspects of your regimen are considered.
Liver Conditions
Q5: How do liver conditions like cirrhosis influence my medication adjustments for the colonoscopy?
"If you're dealing with liver conditions such as cirrhosis, the liver's ability to metabolize medications can be significantly impaired, affecting both the efficacy and safety of the drugs you take."
Adjustment Guidelines:
Reduced Metabolism: Medications that are heavily metabolized by the liver may require dosage adjustments to prevent toxicity.
Bleeding Risks: Cirrhosis often leads to increased bleeding risks, which is critical to manage when preparing for procedures like a colonoscopy.
Action:
Liver Specialist Consultation: Your hepatologist should review your medications to adjust doses or change prescriptions as necessary.
Bleeding Risk Management: Special precautions may be needed, including possibly adjusting or temporarily stopping medications that can exacerbate bleeding.
Diabetes Management
Q6: What changes are needed for my diabetes medications, especially if I'm on insulin or medications like Metformin or Ozempic?
Adjustment Guidelines:
Insulin: You may need to reduce your insulin dosage to prevent hypoglycemia due to decreased food intake.
Oral Diabetics: Medications like Metformin should be reviewed; Metformin is typically paused the day before the procedure to prevent any risk of lactic acidosis, especially as your intake of fluids and solids changes.
Action:
Endocrinologist Review: Have a detailed discussion about your insulin regimen and oral medications in the days leading up to the colonoscopy.
Adjust as Necessary: Your healthcare provider may recommend adjusting the timing and dosage of your diabetes medications to match your prep diet and fasting schedule.
Respiratory Conditions
Q7: Should I adjust my asthma or COPD medications prior to the procedure?.
For those with asthma or COPD, maintaining respiratory stability is crucial, especially right before a medical procedure like a colonoscopy.
Adjustment Guidelines:
Inhalers and Bronchodilators: Typically, you should continue using your inhalers and bronchodilators as normal to ensure that your breathing is not compromised.
Systemic Steroids: If you're on systemic steroids for COPD or severe asthma, these might need adjustment as they can affect immune function and healing.
Action:
Consult Your Pulmonologist: It’s essential to discuss how to use your respiratory medications leading up to the procedure, particularly if you are under sedation.
Medication Review: Bring a list of all respiratory medications to your appointment to ensure all medications are accounted for in your pre-procedure plan.
Autoimmune Disorders
Q8 Do medications for autoimmune disorders require adjustments before a colonoscopy?
Adjusting medications for autoimmune disorders such as rheumatoid arthritis or lupus is vital to manage inflammation and immune response during your colonoscopy.
Adjustment Guidelines:
Immunosuppressants: These may need to be reduced or temporarily halted to balance the risk of infection and inflammation.
Non-Steroidal Anti-Inflammatory Drugs (NSAIDs): Often used in autoimmune disorders, these should generally be stopped several days before to reduce bleeding risks.
Action:
Specialist Consultation: Review your treatment plan with your rheumatologist or immunologist to ensure your autoimmune condition is managed appropriately during the colonoscopy preparation.
Safety and Efficacy: Ensure you understand the implications of any changes in your medication regimen, particularly how they might affect your recovery from the procedure.
Mental Health Conditions
Q9 Can I continue my mental health medications such as antidepressants, anti-anxiety, or mood stabilizers?
Maintaining mental stability is just as important as physical health when preparing for a procedure like a colonoscopy.
Adjustment Guidelines:
Antidepressants and Mood Stabilizers: Generally, you should continue these medications without interruption to avoid withdrawal symptoms or destabilization of your mental health.
Anti-Anxiety Medications: Some sedative anti-anxiety medications may need to be adjusted due to potential interactions with anesthesia drugs used during the colonoscopy.
Action:
Mental Health Provider Review: Discuss any potential interactions with anesthesia and whether dosages need adjustment.
Continuous Care: Ensure there is a plan for post-procedure mental health care, especially if changes to your medication were required.
Supplements and Herbal Adjustments
Q10: Which supplements, vitamins, or herbal remedies should I pause, and when?
As we refine our focus on medications, let's not overlook the impact of supplements and herbal remedies.
Adjustment Guidelines:
Blood-Thinning Supplements: Supplements like fish oil, vitamin E, and ginkgo biloba should be paused as they can increase bleeding risk.
Herbal Remedies: Some herbs can interact with anesthesia or medications used during the procedure, such as St. John's Wort or valerian root.
Action:
Comprehensive Review: Include all your supplements when discussing your medication management plan.
Safe Cessation: Determine the right time to pause these supplements to minimize any impact on the procedure or your recovery.
Emergency Medications
Q11: What emergency medications (e.g., for angina, asthma) should I have on hand, and how should I use them if needed?
Adjustment Guidelines:
Readiness: Keep emergency medications like nitroglycerin for angina or a rescue inhaler for asthma readily accessible.
Instructions: Ensure you and anyone assisting you are clear on how to use these medications if an emergency arises.
Action:
Pre-Procedure Communication: Inform the medical team of all emergency medications you have, including where they are stored and how they should be administered.
Review and Practice: Familiarize yourself and caregivers with the use of these medications under stress to ensure quick and correct usage.
Final Check
Action: Compile a comprehensive list of all your medications, including doses and timing, and review it with your healthcare provider to confirm your medication plan for the days leading up to your colonoscopy
As we close today’s episode on medication adjustments for your upcoming colonoscopy, there’s one last critical step we need to ensure — the final check of your medication list. This step is paramount to safeguarding your health and ensuring the procedure goes smoothly without any medication-related complications.
Detailed Explanation:
The final check involves compiling and reviewing a comprehensive list of all your medications. This list isn't just a formality; it's a crucial component of your pre-procedure preparation. It helps your healthcare team understand exactly what you're taking, so they can make informed decisions about what needs to be paused, adjusted, or continued right up to the day of your colonoscopy.
Actionable Steps:
Compile Your Medication List:
Details to Include: List every medication, including over-the-counter drugs, prescriptions, herbal supplements, and vitamins. For each item, note the dose, the timing of your doses, and any special instructions associated with them.
Consult with Your Healthcare Provider:
Purpose: Review each medication with your doctor or a pre-procedure nurse who specializes in preparing patients for surgery and procedures. This review is critical to identify any potential interactions with the anesthesia or the procedure itself.
Outcome: Your provider may give the green light to continue some medications up to the day of the procedure or might adjust dosages to prevent interactions or side effects.
Documentation:
Update Your List: After the consultation, update your medication list based on the feedback from your healthcare provider.
Keep it Accessible: Make sure this updated list is easily accessible. Bring a copy on the day of your colonoscopy, and consider having a digital copy available on your phone or a health app.
Taking the time to thoroughly review and update your medication list with your healthcare provider is not just about following protocol — it’s about taking active steps to ensure your safety. As you complete this final check, you are setting the stage for a successful and complication-free colonoscopy. Remember, each medication you take has the potential to affect the outcome of your procedure, and being proactive in managing these details is key."
Thank you for tuning in to today’s episode. Next time, we will delve into the 24-hour pre-procedure preparations, discussing everything from your last meals before the procedure to the initiation of your bowel prep. It’s an episode paced with vital information to help you navigate the last crucial steps before your colonoscopy."
Stay prepared, stay informed, and I’ll see you in the next episode of our Colonoscopy Preparation Podcast series. Until then, take care of yourself, and keep that medication list updated and reviewed!
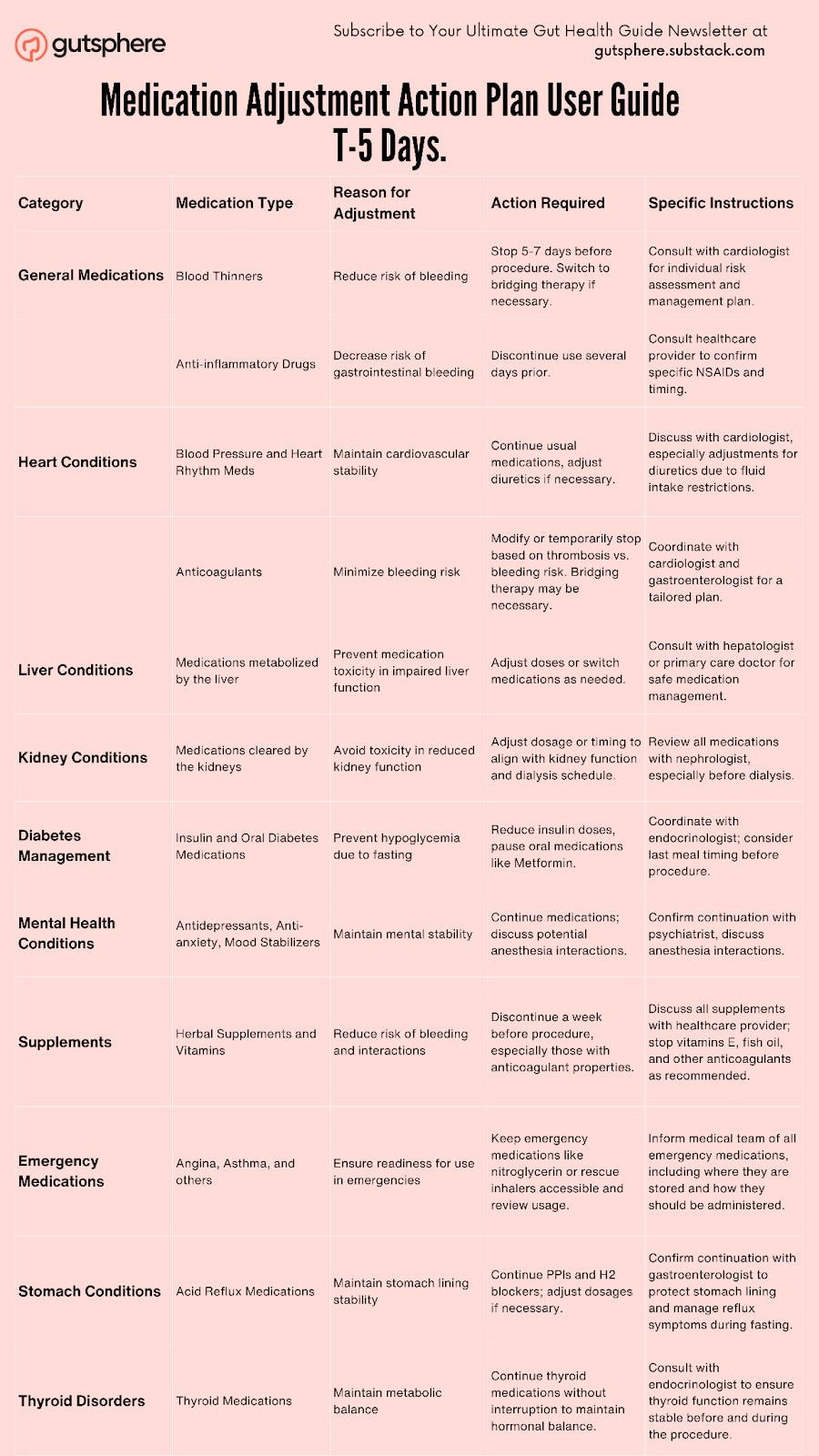
Medication Adjustment Action Plan User Guide
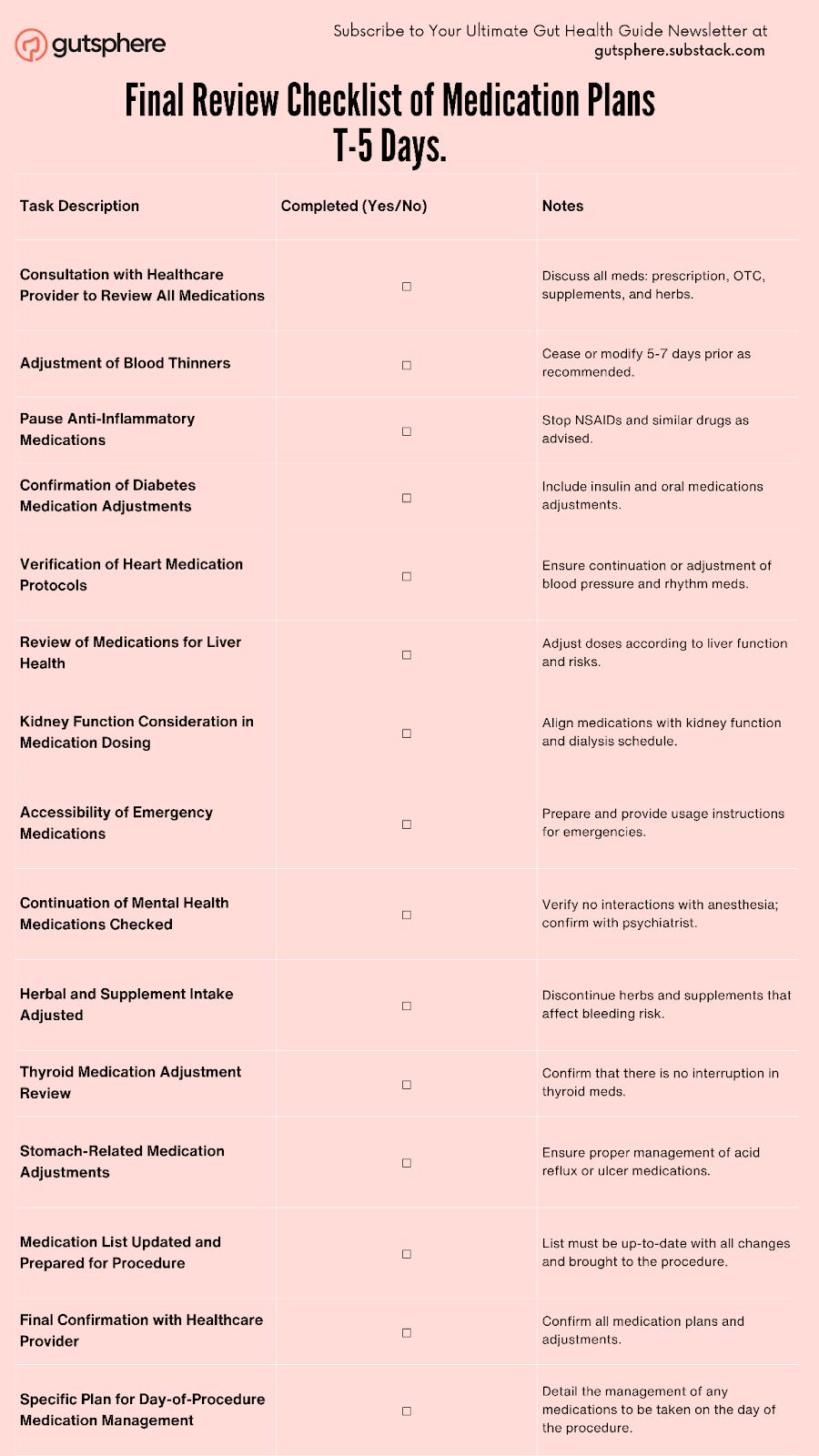
Final Review
Checklist of Medication Plans
Request
Share
Our sincere request to you is to share the newsletter with your friends, family, and community so that they can benefit from the content. Also it will help us grow the newsletter, and eventually, as we release more content, digital tools, and more we will enable people around the world to live chronic disease free.
Subscribe
Feedback
Also, please give us feedback so that we can improve the content. And if there are any topics that you want us to cover please send us your questions and topics. Furthermore, if you try any of the things we provided information please share your experience with us.
Thank You
GutSphere Team
Disclaimer
Please note that the information provided in this newsletter is for informational purposes only and should not be considered as a substitute for professional medical advice, diagnosis, or treatment. If you have any concerns or questions about our health, please consult with a licensed healthcare professional. The information contained in this newsletter is not intended to diagnose, treat, cure, or prevent any disease. The publisher and authors of this newsletter assume no responsibility for any adverse effects that may result from the use of the information contained herein.
References:
General Medication Adjustments:
“Which medications should I adjust, and how, as I approach the colonoscopy date?” 1
“How should I manage over-the-counter medications I typically take for pain, allergies, or sleep?” 1
Heart Conditions:
Kidney Conditions:
“Are there specific considerations for adjusting medications if I have reduced kidney function or am on dialysis?” 3
Liver Conditions:
Diabetes Management:
“What changes are needed for my diabetes medications, especially if I’m on insulin or medications like Metformin or Ozempic?” 5
Respiratory Conditions:
Autoimmune Disorders:
Mental Health Conditions:
“Can I continue my mental health medications such as antidepressants, anti-anxiety, or mood stabilizers?” 7
Supplements and Herbal Adjustments:
Emergency Medications: